Health
Medical Miracles
From stories of personal recovery to advancements in patient care, there’s a lot to celebrate about the southwest Missouri medical community.
by Ettie Berneking
Jul 2021

There’s a lot going in the southwest Missouri medical community that’s worth celebrating. Read the stories listed below to find four inspiring personal experiences of unexpected recovery and three ways the local medical community is working for you through useful tools like expanded mental health services and the rise of the super clinic. Read more in the stories linked below.
Personal Stories

The Big Stressor
How Billie Marsh finally found a solution for her ever-present migraines.

The Three Year Itch
How Candice Reed beat breast cancer and a bug bite infection.

Beating the Odds
How Michael Thompson is still working six years after a dire diagnosis.
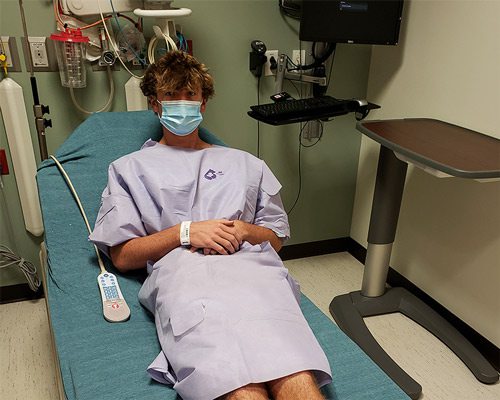
The Team Player
How Rafe Darter came back from a torn ACL to get back into playing sports.
Our Growing Medical Community

Learning in 417-land
How local residencies are helping stave off a future primary care crisis in our community.

On the Move
How CoxHealth is expanding primary care in southwest Missouri with new super clinics.

Creative Thinking
How Burrell Behavioral Health came up with new ways to meet the needs of mental health.