Top Doctors
How Local Hospitals Responded to the COVID-19 Pandemic
An inside look at how CoxHealth, Mercy and other local hospitals made quick decisions and big changes as the COVID-19 pandemic inched its way into the midwest region.
By Ettie Berneking
Jul 2020
Let’s Start With the Numbers
By the end of May, Missouri had reported 11,752 COVID-19 cases and 676 deaths. At press time in Greene County, there were 195 confirmed cases and seven deaths. At CoxHealth, the hospital treated 26 COVID-19 patients total at all of its locations; Mercy Hospital Springfield has had 86 COVID-19 tests come back positive, Citizens Memorial in Bolivar treated 13 cases and Freeman Hospital in Joplin has seen around 100 cases. Compared to other regions in Missouri including St. Louis County, which reported more than 4,200 COVID-19 cases and 345 deaths, southwest Missouri reported far fewer positive cases. “I think we were insulated here in the Midwest,” says Dr. Terrence Coulter, a pulmonologist at CoxHealth. “We had time to prepare.”
The first confirmed COVID-19 case in the United States was reported January 21, and the first case in Greene County wasn’t confirmed until March 12 when a patient sought care at an off-campus CoxHealth clinic in Springfield. For many in southwest Missouri, COVID-19 didn’t seem threatening until it arrived on our doorstep. Even Steve Edwards, the president and CEO of CoxHealth, wasn’t too concerned about COVID-19 when news of the virus started percolating in December. “When northern Italy happened is when I got spooked,” he says.
“I think we were protected here in the midwest. We had time to prepare.”— Dr. Coulter, CoxHealth
By March, American cities were scrambling to find sufficient personal protective equipment (PPE), and community spread of the virus had settled in like a thick fog. The threat of the virus suddenly seemed all too real, and hospitals and health care systems around southwest Missouri were putting disaster plans into place. Dr. Robin Trotman, an infectious diseases physician and medical director of Infection Prevention at CoxHealth, was one of seven doctors added to an advisory committee that updated Governor Mike Parson and state leaders about the current situation and potential vulnerabilities with the state’s health care system. In mid-March, Trotman was meeting with the committee weekly.
Inside hospitals across the Ozarks, elective procedures were put on hold and incident command structures were put in place.
A New Chain of Command
Southwest Missouri has seen its share of disasters. In 2011, an EF5-rated tornado decimated downtown Joplin and killed 158 people. In 2012, Branson was hit by an EF2 tornado, and then in July 2018, the Ride the Ducks tragedy took the lives of 17 riders. During all of these incidents, area hospitals put their incident command structures into effect. “We get people from all over the health system at the table from the supply chain to nursing,” says Paula Baker, president and CEO of Freeman Health System. “We met several times a day initially because things were changing so rapidly. There was no guide book. We had to be very adaptive.”
The incident command structure removes the usual need for routine meetings and committees in order to react quickly and implement new policies in a matter of minutes. “It’s more of a military approach,” Edwards says. “CoxHealth is a 114-year-old organization, so we have a lot of groups that need to have buy-in usually.” Under incident command, the only buy-in needed is from the key team made up of people from the emergency department to the director of infectious diseases.
Initially, hospitals focused on communicating with staff. “To be on the frontlines of a pandemic is frightening,” Baker says. “We focused on communication and worked really hard to prepare our staff, so they understood how to keep themselves safe.” At CoxHealth, Edwards says the daily staff email was bolstered by the addition of a new phone call. There were 600 managers on the call who could ask and answer questions.
The Hunt for PPE
One of the questions being asked was if hospitals had enough PPE. As part of their emergency plans, hospitals across southwest Missouri had put aside PPE including gloves and N95 masks. “We’ve always put some back for pandemic purposes,” says Dr. William Sistrunk, head of infectious disease at Mercy. But as COVID-19 cases overwhelmed hospitals in New York, New Jersey and Detroit, the PPE supply chain couldn’t keep up. “We were hearing there was a shortage,” Sistrunk says. “We realized if this was going to go on for a long time, we were going to need to do things differently to maintain our supply.”
To get a better idea of how quickly area hospitals were using up PPE even in Springfield where the number of positive cases was relatively low, consider this—Edwards says CoxHealth normally used 40 N95 masks a month before COVID. “Now we were using 1,000 masks a day,” he says. Overall, area hospitals didn’t run out of PPE. That’s partly thanks to a healthy stockpile of protective gear and partly thanks to the fact that cases in southwest Missouri were low due to social distancing. But it’s also thanks to some creative problem solving.
To avoid running out of N95 masks, Sistrunk says Mercy is sanitizing and reusing its masks with the help of an Altapure disinfecting system. Masks are hung up on clotheslines in a sealed off room and disinfected before being redistributed. “We worked with the CDC and suppliers to develop this process,” Sistrunk says. “Now it’s being done in a lot of health systems across the country.”
A New Way of Doing Things
Outside of the traditional hospital setting, clinics including Burrell Behavioral Health were also coming up with creative solutions as clinic operations were restricted. “We created a daily Be Well Facebook community,” says C.J. Davis, president and CEO of Burrell. The Be Well program promotes self-care strategies for stress, and so far, 2020 has been incredibly stressful. “For every 1% increase in unemployment, there’s an expected 1.6% increase in suicide,” Davis says. In March 2019, Missouri’s unemployment rate was 3.3%. In March 2020, the unemployment rate jumped to 4.5%. That has Davis worried, and he says Burrell has seen a 20% increase in calls coming in through the center’s crisis line.
“It’s a risk-benefit analysis, but everything is essential to the person who wants it.”— Dr. Robin Trotman, CoxHealth on tough decisions made by hospitals during the pandemic
Even hospitals have had to furlough employees as elective procedures were put on hold. Edwards says Cox delayed some 6,000 surgeries or procedures in just two months. To determine which cases could be postponed, Trotman says each hospital has a committee of surgeons and providers who evaluate upcoming case logs and diagnoses. “It’s a risk-benefit analysis,” he says. “But everything is essential to the person who wants it.”
To reduce furloughs at Mercy Springfield, the hospital was able to reassign many nurses and staff whose workload had been reduced to make face shields. SMC Packaging provided the plastic needed for the face masks, and Lowe’s donated foam while Mercy team members assembled the final products. By the end of May, Mercy had made more than 50,000 plastic face shields. CoxHealth also began creating its own PPE and teamed up with Missouri State University’s Jordan Valley Innovation Center to produce plastic face shields. It even worked with Polyfab Plastics to design a new plexiglass aerosol box that’s placed over a patient’s head as they’re intubated in order to reduce the risk of exposing doctors to the virus.

At Freeman Hospital, Baker says grab-and-go, family-sized meals were made and sold to staff, and an in-house grocery store was set up. “We knew a lot of our staff had extra pressure on them,” she says. “It might not be safe for them to go to the grocery store, so we made groceries available here,” including the elusive toilet paper. Freeman also set up a drive-thru COVID-19 testing site. Like many hospitals and clinics around southwest Missouri, the goal was to keep patients and hospital staff safe by identifying COVID-19 positive cases before they entered the hospital. Anyone who was worried about their symptoms could call into the screening center, and if they met symptom guidelines, they were given a time slot to come through the drive-thru test site.
Baker says some 500 patients have been tested through clinics or the drive-thru test site. “Only 16 tested positive,” she says. “Out of those, five required hospitalization, and 11 recovered at home. All five of the hospitalized patients have recovered.”
Working side by side, CoxHealth, the Greene County Health Department and Mercy assembled a mobile testing site. Mercy and Cox have taken turns staffing the site, and Sistrunk says the site runs 80 to 90 tests a day. “We knew if patients showed up at the hospital with symptoms, we would create an outbreak,” Edwards says. The hope is that the mobile site provides a safe place for patients to be screened for symptoms and sent to the appropriate site for care. For patients without insurance, the mobile site is waiving fees. “We didn’t want any reluctance in the community about testing,” Edwards says.
Inside Mercy’s emergency room, staff set up a COVID-19 triage area to screen patients as they came in. Now Mercy and Cox are working with the Mayo Clinic in a research project using convalescence serum with antibodies from patients who have recovered from COVID-19. The serum is currently being used to treat patients who have recovered from COVID-19 to see if it speeds up recovery.
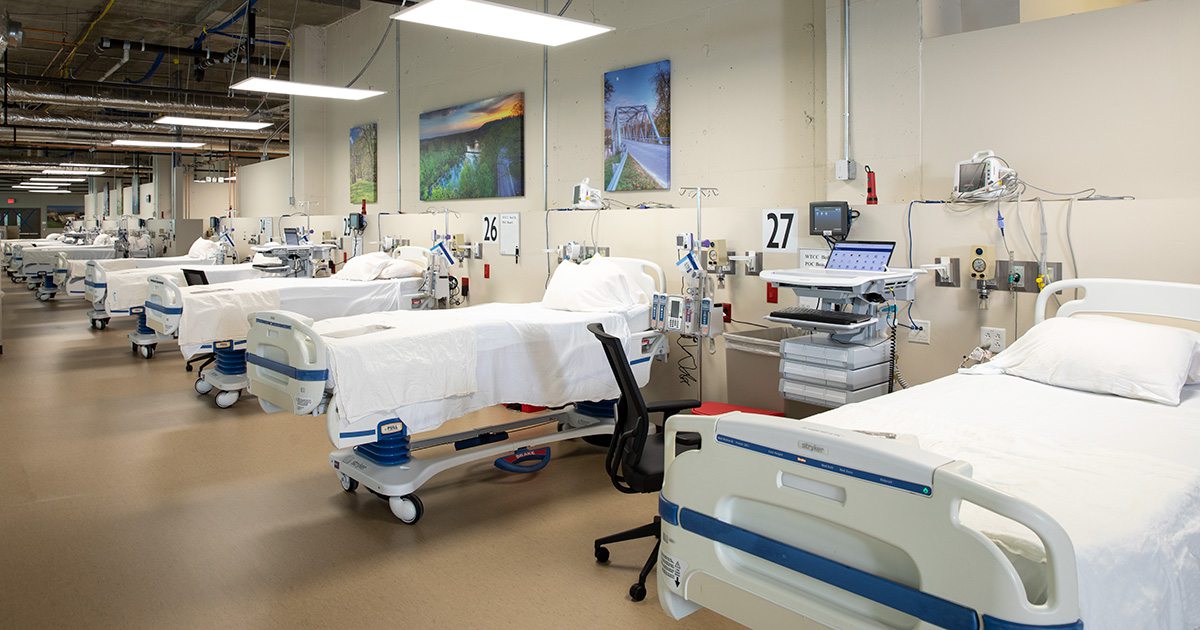
Creating COVID-19 Units
To keep the virus at bay within the hospital, many hospitals set up special COVID-19 units. Initially, Cox set up a triage tent outside the ER to test people with COVID-like symptoms and converted areas within the ER to negative pressure, so air in the room was forced out through a vent to prevent it from circulating around the rest of the hospital. “The concern was transmission,” Edwards says. To prepare the hospital for a possible surge of cases, Cox built a 51-bed ICU to house COVID-19 patients. The project cost $700,000 and took just two weeks to complete. All construction costs were covered by Prime, Inc. To date, the unit hasn’t had to be used, and Edwards is thankful for that. Cox also converted its fifth floor into a non-ICU COVID-19 unit for patients who tested positive and were convalescing or who needed treatment but who weren’t severe enough to need a ventilator.

Hospitals also started running their own COVID-19 tests with many of the test kits coming from private labs. This came about in part due to sheer necessity. “In the first weeks, it took 14 days to get test results,” Edward says, “which was untenable.” Cox and Mercy ended up launching in-house labs and can now get results within 24 hours. “Testing became critical,” Edwards says. So far, Edwards says Cox has run 7,118 tests, Mercy has run 3,600 in-house COVID-19 tests and Citizens Memorial has run 1,933.
Rise of Telemedicine
For patients who didn’t have COVID-related symptoms and who simply needed basic followup care for diabetes, high cholesterol, mental health treatment, prenatal care… you name it, telemedicine has been a lifeline. “Telemedicine has been used in niches in the past, but the pandemic turned everything on a dime,” says Dr. Jennifer McNay, president of Mercy Clinics in Springfield. “We had the ability to reach patients through video, but COVID has forwarded the training on this.”
One of the perks of telemedicine, is its ability to connect patients and physicians without a face-to-face interaction. Patients can be screened for COVID-19 symptoms or report to their doctor about other health issues they’re concerned about without having to leave their home. This has been especially helpful for those at risk patients who need ongoing treatment for chronic illnesses. “It’s been a tremendous resource,” McNay says. Sistrunk estimates COVID-19 pushed Mercy’s telemedicine capabilities forward 10 years.
The rise of telemedicine is especially evident at Burrell where Davis reports no-show rates and cancellations are at an all-time low. “The barriers that were once there, like transportation, are gone,” he says. “You can call the office and be connected with someone in 30 minutes. The convenience and client experience have been dramatically improved.” But it’s not just patients relying on telemedicine, especially for mental health treatment.
“The other group of people impacted are front line workers like health care and EMT workers,” Davis says. “We realized there were a lot of people out there who were experiencing some sort of anxiety related to COVID.” In May, Davis says Burrell was seeing about a 15% increase in service demand. To help health care workers manage stress and find support, Burrell set up a “warm line.” Health care workers can call in and be connected to others in similar situations and receive help from professional counselors. “We also produced videos on coping skills,” Davis says.
“If the community hadn’t done the social distancing or businesses and schools hadn’t closed, we could have had so many patients that would have overwhelmed the health care system.”— Dr. Sistrunk, Mercy
As the stay-at-home order ends and social distancing restrictions are lifted, Davis, Baker, Edwards, Sistrunk, McNay and Trotman all predict there will be more COVID-19 spikes in southwest Missouri. “Predicting is dangerous business right now,” Edwards says, “but unless there is some major interruption to the spread, it’s a serious concern that the virus might be around for up to two years or until we get a vaccine.” That means that for the unpredictable future, hospitals and clinics are leaving COVID units intact.
“We’re going to have to live with this,” Edwards says. “This might go on for a couple of years until the virus runs out of carriers, and the carriers are us.” That might sound alarming, and for good reason when you look at the rising national death toll, but in the Ozarks, health care leaders generally feel prepared. They feel like they’ve had time on their side, in part due to community-wide efforts to stay safe. “If the community hadn’t done the social distancing or businesses and schools hadn’t closed, we could have had so many patients that would have overwhelmed the health care system,” Sistrunk says. “This was a community effort.”